Pemeriksaan Fisik Thorak Dan Abdomen
-
Upload
ahmada-haji -
Category
Documents
-
view
160 -
download
11
Transcript of Pemeriksaan Fisik Thorak Dan Abdomen

Oleh:
Ns. Anis Ika Nur Rohmah
Dalam Perkuliahan Semester Genap Program Studi Ilmu Keperawatan FIKES-UMM

LEARNING OUTCOMES Mahasiswa mampu melakukan
pemeriksaan fisik thorak dan abdomen, secara akurat sebelum dilakukan analisis data, organisasi data, perumusan masalah, serta rencana tindakan keperawatan pada pasien.

Struktur dan fungsi toraks • Tulang toraks terdiri dari 12 vertebra toraksal, 12
pasang iga, klavikula, dan sternum.
• Garis imajiner pada torak:
1. Garis midsternal,
2. Garis midklavikular,
3. Garis aksilaris anterior,
4. Garis aksilaris media,
5. Garis aksilaris posterior,
6. Garis skapularis, dan
7. Garis midspinal.

Pemeriksaan paru Stetoscop
Px.dada posterior pasien posisi duduk, lengan dilipat dan diletakan dipangkuan.
Px. Dada anterior pasien berbaring :
Bila laki-laki dibuka sampai pinggang
Bila perempuan harus menjada privacy area yg sensitif
Menjaga lingkungan yang aman dan nyaman

Auskultasi dinding dada • Stetoskop biasanya mempunyai dua kepala bel
dan diafragma.
• 4 macam bunyi pernapasan normal, yaitu:
• trakeal • vesikuler
• bronkial • bronkovesikuler
• Bunyi pernafasan abnormal :
- Ronchi - Pleural Friction Rub
- Wheezing

Suara Nafas Normal
1. Trakeal : bunyi yang terdengar kasar, keras, dan dengan
tinggi nada tinggi pada bagian trakea ekstratoraks
2. Bronkial : bunyi yang dengan tinggi nada tinggi, seperti udara mengalir melalui pipa didengar di atas manubrium sternal
3. Vesikular : bunyi yang terdengar lemah dengan tinggi nada rendah seluruh lapang paru
4. Bronkovesikular : campuran bunyi bronkial dan bunyi vesikular hanya terdengar pada ICS I dan II


Suara nafas tambahan (Adventitious (Extra) Lung Sounds) Crackles/ Rales : These are high pitched, discontinuous
sounds similar to the sound produced by rubbing your hair between your fingers. signs of water in the alveoli (heart failure), pus in the alveoli (pneumonia), or scarring (pulmonary fibrosis)
Wheezes/Wheezing: These are generally high pitched and "musical" in quality. Stridor is an inspiratory wheeze associated with upper airway obstruction (croup). sign of asthma or, if localized, of a tumor or foreign body
Rhonchi : These often have a "snoring" or "gurgling" quality. Any extra sound that is not a crackle or a wheeze is probably a rhonchi. originate in larger airways than wheezes and are a sign of bronchitis
Friction rub is a dry, leathery sound heard in inspiration and expiration. It is a sign of inflammation of the pleura.

Inspeksi • Wajah pasien; terlihat sianosis, pernapasan cuping
hidung.
• Perhatikan otot-otot bantu napas:
– Suprasternal
– Intercostae
– Sternokleidomastoideus
– Supraclavikula

Bentuk Tulang 1. Bentuk torak :
• Barrel Chest
• Funnel Chest
• Pigeon Chest
2. Bentuk Tulang Belakang
• Kifosis
• Skoliosis
• lordosis

Mengkaji kecepatan dan pola respirasi
Hitunglah frekuensi 30 detik kalikan2, atau dalam 60
detik penuh (N: 12 s/d 20 x/mnt)
Kelaiaanan pola nafas:
Bradipnea
Takepnea
Apnea
Hipernea
Kusmaul
Chanestokes

Palpasi dinding dada posterior
Daerah nyeri tekan
Kesimetrisan pergerakan dada
Fremitus vokal dan fremitus taktil

Perkusi dinding toraks Intensitas Suara:
1. Resonan / sonor
2. Dullness / Pekak
3. Hiperresonan / Hipersonor

Pemeriksaan jantung • Inspeksi keadaan umum pasien
• Penampilan pasien
• Kondisi kulit , ekstremitas inferior lebih dingin dibanding ekstremitas superior (Anemia)
• Kelainan pada wajah dan kepala, Stenosis aorta kongenital (mata berjauhan, strabismus, telinga letak rendah, hidung yang menengadah, dan hipoplasia mandibula), Wajah bulat ,mata terbelalak berjauhan (stenosis pulmonal), kardiomiopati (Lipatan daun telinga/Lichtstein bilateral)
• Mata dapat memperlihatkan arkus senilis (Hipercolesterol)
• Perdarahan konjungtiva (endocarditis)

Palatum yang melengkung tinggi kongenital seperti prolaps katup mitral.
Petekie pada palatum karena endokarditis bakterial.
Pasien dengan defek septum atrium mungkin mempunyai falang ekstra, jari tangan ekstra, atau jari kaki ekstra. Jari tangan yang panjang dan kurus mengarah kepada kemungkinan regurgitasi aorta.

Perkusi batas-batas jantung • Pada kondisi normal akan didapatkan bunyi redup
pada :
- ICS (Intercostal Space) II midsternalis kiri
(batas atas),
- ICS (Intercostae Space) V (batas bawah),
- Midklavikula kiri (batas kiri), dan
- ICS (Intercostal Space) II dekstra midsternalis
kanan (batas kanan).

PERCUSION A. Proper Technique
1. Hyperextend the middle finger of one hand and place the distal interphalangeal joint firmly against the patient's chest.
2. With the end (not the pad) of the opposite middle finger, use a quick flick of the wrist to strike first finger.
3. Categorize what you hear as normal, dull, or hyperresonant.
4. Practice your technique until you can consistantly produce a "normal" percussion note on your (presumably normal) partner before you work with patients.
B. Posterior Chest 1. Percuss from side to side and top to bottom using the
pattern shown in the illustration. Omit the areas covered by the scapulae.
2. Compare one side to the other looking for asymmetry.
3. Note the location and quality of the percussion sounds you hear.
4. Find the level of the diaphragmatic dullness on both sides.

Interpretation
C. Anterior Chest 1. Percuss from side to side
and top to bottom using the pattern shown in the illustration.
2. Compare one side to the other looking for asymmetry.
3. Note the location and quality of the percussion sounds you hear.
Percussion Notes and Their
Meaning
Flat or
Dullness liquid or solid 1. Pleural Effusion
2. Lobar Pneumonia
lung area full of pus
Normal Healthy Lung or
Bronchitis
Hyperresonant Emphysema or
Pneumothorax

PALPATION 1. Identify any areas of tenderness or deformity by
palpating the ribs and sternum Daerah nyeri tekan
2. Assess expansion and symmetry of the chest by placing your hands on the patient's back, thumbs together at the midline, and ask them to breath deeply. Kesimetrisan pergerakan dada
Vokal Fremitus dan Fremitus taktil

Tactile fremitus: Chest wall vibrations from speech (patient says "ninety-nine").
Compare sides. Fremitus should be symmetric - the same on both sides.
Abnormal fremitus can help you diagnose several lung abnormalities:
Decreased fremitus occurs if something gets between the lung and chest wall:
Air in the pleural space ( pneumothorax or "collapsed lung")
Fluid in the pleural space (pleural effusion)
Scarred, thickened pleura Increased fremitus: In pneumonia, thick pus in the airways
and alveoli increases vibration transmission (like wobbling jello). Patients with pneumonia may have increased fremitus on that side.

Auskultasi jantung • Cara yang paling dapat diandalkan untuk mengenali Sl dan
S2 adalah menentukan waktu terjadinya bunyi itu dengan palpasi arteri karotis.
• Sementara tangan kanan pemeriksa mengubah-ubah posisi stetoskop, tangan kiri diletakkan pada arteri karotis pasien. Bunyi yang mendahului denyut karotis adalah S1. Sedangkan S2 terdengar setelah denyut tersebut.
• Ketika mendengarkan pada apeks dan batas sternal kiri dengan bel stetoskop, pemeriksa harus menentukan apakah ada bunyi jantung III (S3) atau tidak.

Pemeriksaan bising jantung
• waktu dalam siklus jantung • tinggi nada
• lokasi dan penyebaran • kualitas
• intensitas

SUARA UCAPAN
1. Bronchophony is increased clarity of words, e.g. in area of pneumonia
2. Whispered pectoriloquy -- even a whisper is clear to the stethoscope - is an extreme form of bronchophony (Suara terdengar jauh dan tidak jelas)
3. Egophony: patient says EE and stethoscope hears A - is similar to increased tactile fremitus. Egophony may be the only physical examination abnormality in early pneumonia.

JANTUNG/CARDIO Examination of the heart includes: • Inspection: of jugular venous pulse and point of maximal impulse • Palpation: of point of maximum impulse, and precordium for lifts, heaves and thrills • Auscultation: for valve closing sounds (S1 and S2), extra sounds (S3 and S4), murmurs, clicks and rubs

PEMERIKSAAN ABDOMEN

1. The patient should have an empty bladder. 2. The patient should be lying supine on the exam table and
appropriately draped. 3. The examination room must be quiet to perform adequate
auscultation and percussion. 4. Watch the patient's face for signs of discomfort during the
examination. 5. Use the appropriate terminology to locate your findings 6. Disorders in the chest will often manifest with abdominal
symptoms. It is always wise to examine the chest when evaluating an abdominal complaint.
7. Consider the inguinal/rectal examination in males. Consider the pelvic/rectal examination in females.
EXAM SECTIONS 1. Inspection 2. Auscultation 3. Percussion 4. Palpation
General Considerations

1. INSPECTION
Physicians locate findings in the abdomen in one of four quadrants or one of nine regions.
The four quadrants are: right upper (RUQ), right lower (RLQ), left upper (LUQ) and left lower (LLQ). THE NINE REGIONS epigastric, umbilical, hypogastric/suprapubic, right hypochondriac, left hypochondriac, right lumbar, left lumbar, right inguinal and left inguinal.

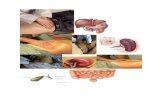
LOCATIONS of ABDOMINAL ORGANS
The schematic below is a reminder of what organs are likely to produce findings in each region. For example: Right hypochondriac (RUQ) : liver and gall
bladder left hypochondriac (LUQ) : the spleen and
stomach epigastric : the pancreas, stomach and
common bile duct umbilical : the small intestine lumbar : the kidneys iliac regions : the ovaries left iliac/LLQ : the sigmoid colon right iliac or lumbar (RLQ): the cecum and
appendix suprapubic : the bladder and uterus

SOME COMMON FINDINGS on ABDOMINAL INSPECTION Scars : Jaringan parut
Striae (stretch marks) : tanda peregangan ibu hamil
Colors : - Bluish color at the umbilicus is Cullen's sign – a sign of bleeding in the peritoneum.
- Bruises on the flanks are Grey Turner's sign (retroperitoneal bleeding - e.g. from inflamed pancreas)
Jaundice : warna kuning pada kulit
Prominent veins : may be due to portal vein obstruction or inferior vena cava obstruction

ABDOMINAL DISTENSION Distension of the lower abdomen only can be caused by pregnancy, full bladder, ovarian tumor, or uterine fibroids (common benign growths) Diffuse abdominal distension can be caused by any of the 6 Fs: Fat (obesity) Fluid (ascites - peritoneal fluid - or obstructed viscera
filled with fluid) Flatus (air) - e.g. from air swallowing or intestinal
obstruction Feces (constipation Fetus (pregnancy) Fatal cancer.

2. AUSCULTATION GUT SOUNDS
Use the diaphragm of your stethoscope to listen to gut sounds Normal gut sounds are gurgling, 5 to 35 per minute Borborygmi are loud, easily audible sounds. They are normal, too. High pitched , tinkling (raindrops in a barrel) sounds are a sign of
early intestinal obstruction Decreased sounds: (none for a minute) are a sign of decreased gut
activity. Gut sounds may be markedly decreased after abdominal surgery; abdominal infection (peritonitis) or injury.
Absent Sounds : (no sounds for 5 minutes) are a bad sign. They can be caused by longer-lasting intestinal obstruction, intestinal perforation or intestinal (mesenteric) ischemia or infarction

3. PERCUSSION What it finds: liver size (kind of), spleen, fluid.
Percussing the body gives one of three notes:
Tympany is found in most of the abdomen, caused by air in the gut. It has a higher pitch than the lung.
Resonance is found in normal lung. It is lower pitched and hollow.
Dullness is a flat sound, without echoes. The liver and spleen, and fluid in the peritoneum (ascites: ah-SY-teez), give a dull note.

A. Liver Span Percuss downward from the chest in the right midclavicular line
until you detect the top edge of liver dullness. Percuss upward from the abdomen in the same line until you detect
the bottom edge of liver dullness. Measure the liver span between these two points. This measurement
should be 6-12 cm in a normal adult.
B. Splenic Dullness Percuss the lowest costal interspace in the left anterior axillary line.
This area is normally tympanitic. Ask the patient to take a deep breath and percuss this area again.
Dullness in this area is a sign of splenic enlargement.

Shifting Dullness This is a test for peritoneal fluid (ascites). ++ Percuss the patient's abdomen to outline areas of dullness and tympany. Have the patient roll away from you. Percuss and again outline areas of dullness and tympany. If the dullness has
shifted to areas of prior tympany, the patient may have excess peritoneal fluid. Psoas Sign This is a test for appendicitis. ++ Place your hand above the patient's right knee. Ask the patient to flex the right hip against resistance. Increased abdominal pain indicates a positive psoas sign. Obturator Sign This is a test for appendicitis. ++ Raise the patient's right leg with the knee flexed. Rotate the leg internally at the hip. Increased abdominal pain indicates a positive obturator sign.

4. PALPATION General Palpation 1. Begin with light palpation.
At this point you are mostly looking for areas of tenderness. The most sensitive indicator of tenderness is the patient's facial expression (so watch the patient's face, not your hands). Voluntary or involuntary guarding may also be present.
2. Proceed to deep palpation after surveying the abdomen lightly. Try to identify abdominal masses or areas of deep tenderness

Palpasi Lien
Posis pasien tetap telentang, buatlah garis bayangan Schuffner ari midclavikula kiri ke arcus costae- melalui umbilicus – berakhir pada SIAS kemudian garis dari arcus costae ke SIAS di bagi delapan. Dengan Bimanual lakukan palpasi dan diskrisikan nyeri tekan terletak pada garis Scuffner ke berapa ? ( menunjukan pembesaran lien )

Palpasi Hepar
Atur posisi pasien telentang dan kaki ditekuk
Perawat berdiri di sebelah kanan klien, dan meletakan tangan di bawah arcus costai 12, pada saat isnpirasi lakukan palpasi dan diskripsikan :
Ada atau tidak nyeri tekan, ada atau tidak pembesaran berapa jari dari arcus costae, perabaan keras atau lunak, permukaan halus atau berbenjol-benjol, tepi hepar tumpul atau tajam. Normalnya hepar tidak teraba.

Palpasi Ginjal
Dengan bimanual tangan kiri mengangkat ginjal ke anterior pada area lumbal posterior, tangan kanan diletakan pada bawah arcus costae, kemudian lakukan palpasi dan diskripsikan adakah nyeri tekan, bentuk dan ukuran.
Normalnya ginjal tidak teraba.

Palpasi Appendik
Posisi pasien tetap telentang, Buatlah garis bayangan untuk menentukan titik Mc. Burney yaitu dengan cara menarik garis bayangan dari umbilicus ke SIAS dan bagi menjadi 3 bagian. Tekan pada sepertiga luar titik Mc Burney : Bila ada nyeri tekan ,nyeri lepas dan nyeri menjalar kontralateral berarti ada peradangan pada appendik.

ANY QUESTION?